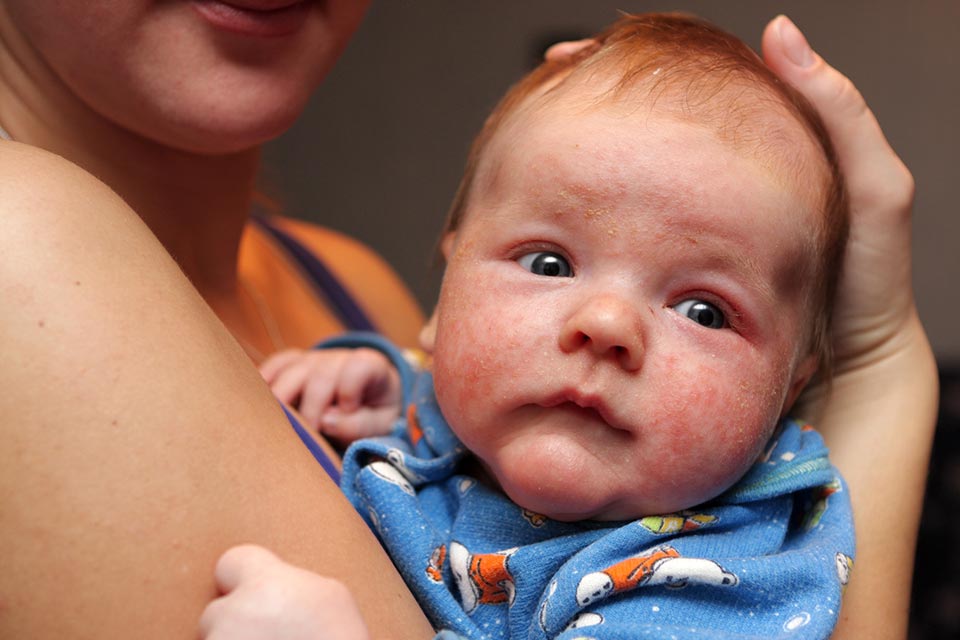
The rash of atopic dermatitis or eczema in the pediatric patient is usually mild in nature. Typically it begins with cradle cap (a scaly rash on the scalp) that appears after birth and looks like dandruff. After a few months some itchiness and redness in the folds of the elbow and knee appear. The child often scratches to the dismay of the parents and an array of foods are incriminated but this is faulty thinking.
We often refuse to accept an idea merely because the tone of voice in which it has been expressed is unsympathetic to us.
The skin is often dry which worsens during the colder winter months with low humid atmospheres increasing the dryness. These are mild symptoms and signs that only need lubrication to benefit the child. As better sunny weather occurs, some outside carefully timed sun exposure is very helpful. A minor amount of rash might have to be tolerated.
If the rash is more severe and the itching is unabated then I recommend very short-term use of a moderately strong corticosteroid cream. A moderate strength steroid requires only 5 – 7 days of usage. Treatment can be repeated days to weeks later if reoccurrence occurs.
Too often the practitioner and/or the parents use very low strength hydrocortisone that undershoots the mark, gives only a small amount of relief, and facilitates the process of addiction. It is the prolonged usage of the low dose steroids necessitated because their results are so minimal that are problematic. Continual daily usage should always be avoided.